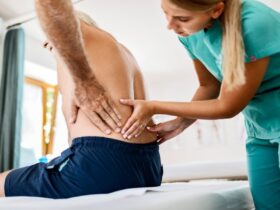
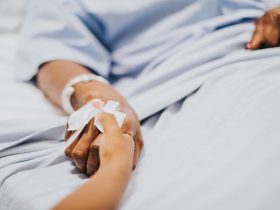
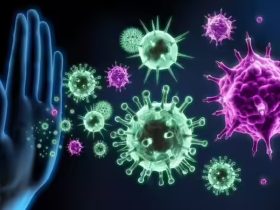
Imagine a persistent, maddening urge to scratch, yet your skin appears completely normal. This is the reality for individuals with a complex clinical entity where itching occurs without primary lesions.
This disorder sits at the crossroads of dermatology and psychiatry. Psychological factors are central to its presentation, often triggering or worsening the distressing sensation.
For those affected, it represents a significant challenge. The lack of a visible cause can lead to frustration and misdiagnosis. Healthcare professionals also find it a difficult puzzle to solve.
Despite its impact, awareness is surprisingly low. A 2017 review found only 62 relevant studies in a major medical database. This highlights a gap in both research and clinical recognition.
This article provides a comprehensive guide. It will trace the understanding of this issue from historical views to modern treatment strategies. The goal is to offer a complete resource for patients and clinicians alike.
The terminology can be confusing. It is also referred to as somatoform pruritus or functional itch disorder. Establishing clear language is crucial for effective discussion and care.
Key Takeaways
- This is a distinct condition characterised by a compelling itch in the absence of visible primary skin disease.
- Psychological and emotional factors play an evident role in starting, intensifying, or continuing the symptoms.
- It presents a significant diagnostic challenge, requiring input from both dermatological and psychiatric specialities.
- The disorder is under-researched, with very limited published literature available to guide practice.
- Multiple terms, including functional pruritus and somatoform pruritus, describe the same core clinical picture.
- Effective management strategies must address both the physical sensation and its psychological contributors.
- Increased recognition amongst healthcare professionals is vital for improving patient outcomes and care.
Understanding Psychogenic Itch: Definition and Overview
An unpleasant sensation provoking a need to scratch, yet with unremarkable skin examination, signals a functional issue. The French Psycho-Dermatology Group (FPDG) formally defines it as “an itch disorder where itch is at the centre of the symptomatology and where psychological factors play an evident role.” They propose the name functional itch disorder.
What is Psychogenic Itch?
This condition is a recognised category within the International Forum for the Study of Itch’s classification. It sits alongside dermatological, systemic, and neurological origins. The core sensation of pruritus has been defined the same way for centuries.
It is an urge to scratch that affects the skin and some mucosa. Importantly, it is distinct from pain, though both may involve burning or tingling.
Key Differentiators from Other Itch Disorders
The primary distinction is the absence of primary skin lesions, known as pruritus sine materia. Other disorders typically have a clear physical cause.
Here, psychological factors are central to triggering or worsening the symptoms. This makes it a positive diagnosis, not just a label after ruling other things out.
Terms like somatoform pruritus are also used. Accurate identification requires noting both the lack of somatic causes and the clinical link to mental state.
Historical Perspectives and Diagnostic Evolution
The journey to recognise functional itch as a legitimate diagnosis has been marked by diagnostic oversights and patient suffering. In past decades, physicians often proposed this label too readily. Patients were rarely referred for psychiatric assessment despite the psychological label.
This haste had severe consequences. Historical cases exist where individuals endured years of misdiagnosis. Serious conditions like Hodgkin’s disease were missed. This highlights the critical need to exclude organic causes thoroughly.
Psychiatric classification systems have evolved significantly. The DSM-IV listed the condition under several somatoform disorders. The DSM-5 later introduced ‘somatic symptom and related disorders’. This change aimed to better reflect mind-body interactions.
The ICD-10 system also classified it under ‘other somatoform disorders’. Specialist groups, like the French Psycho-Dermatology Group, advanced formal definitions. Their work moved the field beyond simple exclusion.
| Era | Diagnostic Approach | Primary Consequence |
|---|---|---|
| Early-Mid 20th Century | Unexplained itch dismissed as ‘nerves’ or hysteria. | Delayed identification of systemic diseases; patient distress. |
| Late 20th Century (DSM-IV) | Categorised within multiple somatoform disorder categories. | Diagnostic overlap and confusion in clinical practice. |
| 21st Century (DSM-5/IFSI) | Positive criteria required; focus on somatic symptom disorders. | More nuanced, integrated understanding of aetiology. |
Modern frameworks now demand both negative and positive diagnostic features. This shift reflects a more sophisticated understanding. It ensures patients receive appropriate, dual-specialty care.
Epidemiology and Impact on Quality of Life
Epidemiological data reveals the scale of the problem and its profound consequences for those affected. Research indicates a notable prevalence and a severe impact on overall wellbeing.
Prevalence and Demographics
One specialised study found roughly 6.5% of dermatology outpatients had somatoform pruritus. This figure may be higher in psychosomatic clinics.
Itch is a common symptom overall. About one-third of people experience it weekly. Ten percent require treatment for the sensation.
Generalised itch without a clear skin cause affects nearly 17% of adults. The prevalence rises dramatically with age, potentially exceeding 50% in the elderly.
Psychological and Physical Burden
The toll on quality of life is substantial. A large survey of 4,995 participants showed a stark contrast.
Sixty percent of those reporting itch had a significant life impact. This compared to just 25% of individuals without the symptom.
The negative effect on health-related quality of life intensifies with the strength of the pruritus. Research consistently links higher itch scores with elevated depression scores.
This creates a difficult cycle. Anxiety and stress can both result from and worsen the itching. For some patients, this leads to severe psychiatric issues, including suicidal thoughts.
Chronic pruritus disrupts life in multiple ways:
- Severe sleep disturbance
- Impaired concentration and work performance
- Social withdrawal and relationship strain
- Persistent low mood and depression
Diagnostic Approaches and Differential Diagnosis
A structured diagnostic framework is essential to accurately identify the source of unexplained chronic pruritus. This process safeguards against misdiagnosis.
Ruling Out Somatic Causes
A thorough physical examination is the first step. It must include a complete dermatologic assessment of the skin.
For generalised itch without obvious cause, standard screening is mandatory. This includes full blood count with ferritin, CRP, and routine biochemistry. Tests cover renal, hepatic, thyroid, and bone function.
Additional investigations like antimitochondrial antibody, urinalysis, chest X-ray, and LDH are often needed. This exhaustive approach rules out systemic diseases such as liver or kidney disorders.
Essential Diagnostic Criteria
The French Psycho-Dermatology Group proposes ten criteria for functional itch disorder. Three are compulsory.
First, localised or generalised pruritus sine materia. Second, chronic duration exceeding six weeks. Third, no somatic cause found.
At least three of seven optional criteria must also be present. These link the itch to psychological factors.
Examples include a chronological relationship with life events or variation with stress. Response to psychotropic drugs or psychotherapy also counts.
This positive identification distinguishes it from idiopathic pruritus. It is not a diagnosis of exclusion.
In-depth Analysis of Psychogenic Pruritus Explained: Managing Itch Without Visible Skin Disease
A biopsychosocial model offers the most accurate lens for analysing this distressing phenomenon. It moves beyond outdated mind-body splits. The core challenge is a compelling itch on clinically normal skin.
In reality, purely ‘psychogenic’ or ‘organic’ presentations are rare. For most patients, a primary somatic disease exists. Their symptoms are then modulated by psychological factors like stress.
In a distinct subgroup, psychological elements are the primary cause of the pruritus. The burden of this condition is immense. It ravages sleep, work, and social bonds for those affected.
How to best classify and understand it remains actively debated. Modern science sees neurophysiological and psychological theories as complementary. Effective management therefore must combine pharmacological treatment with psychological support, a fundamental shift in dermatology.
Expert Insights: Perspectives from The Psychodermatologist
Navigating the gap between dermatology and psychiatry requires a specialist with dual training and insight. The Psychodermatologist provides this crucial bridge, offering comprehensive care for people whose itch originates at the intersection of skin and mind.
Individuals typically consult a dermatologist first, associating the sensation purely with the skin. This often leads to resistance towards psychiatric referral due to stigma. Experts note this creates a diagnostic blind spot.
Psychiatrists seldom encounter these patients, so they may view the condition as very rare. Conversely, many dermatologists readily propose the diagnosis but may lack specific psychological therapy skills.
| Aspect | Dermatologist Perspective | Psychiatrist Perspective |
|---|---|---|
| Typical Patient Encounter | Frequent; first point of contact for unexplained pruritus. | Infrequent; patients often avoid referral. |
| Common Perception | A recognised clinical reality requiring management. | Considered a rare presentation. |
| Primary Expertise | Excluding organic skin and systemic disease. | Assessing and treating psychological contributors. |
| Collaborative Need | Essential for holistic treatment. | Vital for accurate diagnosis and care. |
The expert approach emphasises validation and a non-confrontational style. Thoroughly excluding physical causes builds trust. Introducing psychological factors is done gradually to maintain a strong therapeutic alliance.
Multidisciplinary collaboration is fundamental. Groups like the French Psycho-Dermatology Group model this, combining dermatological and psychiatric competence. In the UK, closer ties between specialities are needed to improve outcomes.
Neurophysiological Underpinnings and Brain-Skin Interactions
Modern neuroscience reveals that the sensation of itching is a whole-brain event, not a simple skin signal. The perception involves cooperation between sensory, motor, and affective brain areas. A region called the precuneus plays a specific role.
This complex network generates the complete experience, including the urge to scratch.
Central Sensitisation and Itch Transmission
Specialised nerve endings, called pruriceptors, are located in the skin. They detect stimuli and send signals via specific pathways to the brain. Research identifies at least two main routes for this transmission.
One is a histaminergic pathway. The other is a non-histaminergic pathway, often dependent on PAR-2. Chronic signalling can lead to central sensitisation.
This alters central nervous system processing, amplifying the sensation over time. Gate control mechanisms, similar to those in pain, can also modulate these signals.
| Pathway Type | Key Mediator | Response to Antihistamines | Clinical Relevance |
|---|---|---|---|
| Histaminergic | Histamine | Often Responsive | Classic allergic or urticarial pruritus |
| Non-Histaminergic | PAR-2, other peptides | Typically Unresponsive | Many chronic and systemic forms of itch |
Role of Neurotransmitters in Itch
Specific brain chemicals are also implicated. The opioid system, acetylcholine, and dopamine are involved in itch influenced by psychological state.
This explains mentally-induced itch. Attention, expectation, or stress can activate the relevant brain regions. This produces a genuine sensation without any peripheral trigger.
This evidence supports a fundamental shift. As researchers note, it is the brain that itches, not the skin. This validates the experience as a real neurological event.
Psychological Factors Influencing Itch Intensity
Mental and emotional states serve as critical amplifiers or dampeners of pruritic sensations. Research confirms a bidirectional relationship where psychological factors influence itch perception, while the symptoms themselves worsen mental wellbeing.
Stress acts as a primary modulator, activating neurobiological pathways that lower itch thresholds. Both acute and chronic stress can amplify existing sensations or trigger new episodes. Anxiety contributes through hypervigilance, where increased attention to bodily sensations heightens perceived intensity.
The interplay with depression is particularly complex. Studies show patients with higher depression scores report more severe itch. This creates a vicious cycle where chronic pruritus worsens low mood, which in turn intensifies the condition.
Major life events often correlate with symptom onset or exacerbation. Bereavement, relationship difficulties, or occupational stress can precipitate itching. Cognitive styles, including catastrophic thinking, further modulate how a patient experiences these sensations.
| Psychological Factor | Primary Mechanism | Effect on Itch Perception | Clinical Note |
|---|---|---|---|
| Stress | Activates HPA axis, releases cortisol and neuropeptides | Lowers threshold, amplifies signal | Both cause and consequence of chronic itch |
| Anxiety | Creates hypervigilance and anticipatory fear | Heightens attention to sensations | Can trigger episodes through psychophysiological response |
| Depression | Alters neurotransmitter balance (serotonin, norepinephrine) | Increases perceived intensity | Bidirectional relationship well-established in research |
Contemporary Treatment Approaches and Management Strategies
Contemporary clinical strategies for unexplained itching integrate medication with behavioural techniques. A combined approach addressing both the physical sensation and its psychological drivers offers the most effective treatment for patients. This evidence-based management is tailored to the UK healthcare context.
Pharmacological Treatments
Topical agents are initial treatment options. Menthol 1-2% in aqueous cream cools the skin. Doxepin 5% cream or capsaicin 0.075% can help localised itch.
Patients may trial oral antihistamines like fexofenadine (180 mg) or loratadine (10 mg) for four weeks. Sedative options include cetirizine (10 mg). Discontinue if ineffective.
Neuromodulators like gabapentin and pregabalin require longer trials. Start gabapentin at 100 mg once daily, titrating to 300-600 mg three times daily. Pregabalin begins at 75 mg twice daily, increasing to 150 mg twice daily. Assess after six weeks.
Psychotropic medications show efficacy for chronic pruritus. Selective serotonin reuptake inhibitors (SSRIs) and mirtazapine are options. For severe cases, low-dose risperidone may be considered under specialist supervision.
Psychological and Behavioural Interventions
Cognitive behavioural therapy (CBT) breaks the itch-scratch cycle. It addresses maladaptive thoughts and promotes coping strategies.
Habit reversal training increases awareness of scratching behaviour triggered by itching. Patients learn competing responses to reduce skin damage.
Integrative care combines medication with psychological support. Multimodal strategies improve treatment response for chronic symptoms. Each patient requires individualised planning.
Adjunctive therapies include stress management, mindfulness, and relaxation techniques. These support overall treatment plans.
Role of Surgical Arena Ltd in Advancing Pruritus Management
Organisational support plays a pivotal role in translating scientific understanding into improved patient outcomes for challenging itch disorders. Entities like Surgical Arena Ltd contribute significantly to this field. They help bridge the gap between complex research and practical clinical care.
Their work supports healthcare professionals in delivering evidence-based treatment. This is vital for conditions where a standard approach is not always clear. They facilitate access to specialist expertise and contemporary protocols.
A key contribution is promoting integrated care models. These models encourage collaboration between dermatology, psychiatry, and primary care. This multidisciplinary strategy is essential for optimising results for patients.
Educational initiatives are another important focus. Professional development resources enhance clinician skills in recognising and managing complex pruritus. This builds competence across the healthcare system.
The organisation also aids in disseminating research and clinical best practices. This supports treatment plans that combine pharmacological and psychological methods. A holistic, patient-centred approach is therefore strengthened.
Ultimately, such efforts validate the patient experience. They foster comprehensive assessment and non-stigmatising communication. This improves the overall management landscape for distressing itch conditions.
Integrative Care: Combining Dermatology and Psychological Support
Successful outcomes in these complex cases often hinge on a coordinated, multidisciplinary approach. This model blends dermatological and psychiatric expertise to tackle both the physical sensation and its psychological roots.
Integrative frameworks are vital for effective care. They validate the individual’s experience while providing a structured path forward.
Multidisciplinary Treatment Plans
An optimal team includes a dermatologist, psychiatrist, psychologist, and a specialist nurse. The general practitioner coordinates ongoing health support.
The process starts with a thorough dermatological assessment to exclude somatic disease. A psychological evaluation follows. This dual approach informs a unified treatment strategy.
Specialist psychodermatology clinics, like those modelled by the French group, are ideal. In the UK, such services are limited. Alternative care models must be considered.
| Care Model | Team Composition | Key Advantage | Consideration |
|---|---|---|---|
| Ideal Psychodermatology Clinic | Dermatologist, Psychiatrist, Psychologist, Nurse | Seamless, co-located expertise | Limited geographic availability |
| Shared Care Protocol | Dermatology & Psychiatry depts. liaising | Formalised communication channels | Requires clear local guidelines |
| Enhanced Primary Care | GP with specialist advice & psychology input | Accessible, patient-centred | Depends on local service provision |
Case Studies and Clinical Observations
Anonymised cases illustrate these principles in practice.
Patient A presented with chronic generalised itch. All organic causes were excluded. Assessment revealed significant anxiety linked to work stress.
Treatment combined an SSRI medication with cognitive behavioural therapy. The patient‘s acceptance of the psychological formulation was crucial. A strong therapeutic alliance supported their progress.
Patient B was initially managed for suspected functional pruritus. Months later, new systemic symptoms emerged. Further investigation revealed an underlying haematological condition.
This case underscores the need for ongoing vigilance. It highlights that initial psychological management does not preclude later organic diagnosis.
Clinical observations show that matching interventions to psychological profiles improves outcomes. Gentle introduction of psychological concepts maintains engagement. This is key for patients managing these distressing disorders.
Practical Tips for Daily Itch Management
Effective management of chronic itching involves both proactive skincare and mindful behavioural adjustments. This section offers actionable guidance for individuals and clinicians to implement immediately.
Lifestyle and Skincare Routine
Liberal, regular use of emollients is fundamental. For very dry skin, especially in older people, an ointment-based moisturiser provides superior barrier protection.
Limit bathing frequency and duration. Use lukewarm water and avoid harsh soaps. Apply moisturiser to slightly damp skin after washing to lock in hydration.
Identify and avoid contact irritants. These include rough textiles, biological detergents, perfumes, and certain chemicals. Wearing smooth, natural-fibre clothing can help.
Cooling topical agents offer relief. A preparation containing 1-2% menthol in aqueous cream can be very soothing when applied to affected areas.
Environmental modifications also matter. Maintain comfortable humidity levels at home. Use hypoallergenic bedding and avoid overheating.
Stress Management Techniques
Psychological factors can intensify the sensation. Regular practice of stress reduction techniques is therefore valuable.
Progressive muscle relaxation, diaphragmatic breathing, and mindfulness meditation can lower overall stress levels. This may reduce itch exacerbations.
Good sleep hygiene is crucial if symptoms worsen at night. Establish a consistent schedule. Keep nails short and consider wearing cotton gloves to bed to minimise skin damage.
Behavioural strategies help break the itch-scratch cycle. Develop awareness of scratching urges. Practice a competing response, like applying a cold compress, instead.
Keeping a symptom diary can identify personal triggers. Regular physical activity also helps by reducing stress and providing a healthy distraction.
Conclusion
In summary, addressing chronic itching rooted in psychological factors demands a holistic framework. This bridges medical and mental health disciplines effectively.
The condition is a legitimate clinical entity where mental state influences physical sensation. It places a substantial burden on patients, affecting sleep, work, and social wellbeing.
Comprehensive care must integrate thorough diagnosis with tailored treatment plans. Effective management combines pharmacological options with psychological therapies.
Moving forward, increased clinician education and ongoing studies are crucial. Advances in neuroscience promise deeper understanding of these complex disorders.
Ultimately, collaboration between dermatology and psychiatry offers the best hope. It optimises health outcomes and quality of life for those affected.